Chronic kidney disease study reveals significant health burden
21 June 2022
People with longstanding kidney disease face health issues like heart disease and diabetes that could impact their risk of severe COVID-19 and life expectancy, according to a new study enabled by the BHF Data Science Centre. The findings could inform treatment pathways for kidney patients during and beyond the pandemic.
The researchers behind the findings say that people living with kidney disease should be prioritised for measures such as vaccination and shielding in the future.
The team led by Professor Amitava Banerjee, a consultant cardiologist and Chair in clinical data science at University College London (UCL), analysed health records from almost 57 million people that linked information from GPs and hospitals. Within this, they identified 2.3 million people aged 30 and over who either had a history of chronic kidney disease or developed the condition during the pandemic. These patients’ records were followed up from 1997 to 2021.
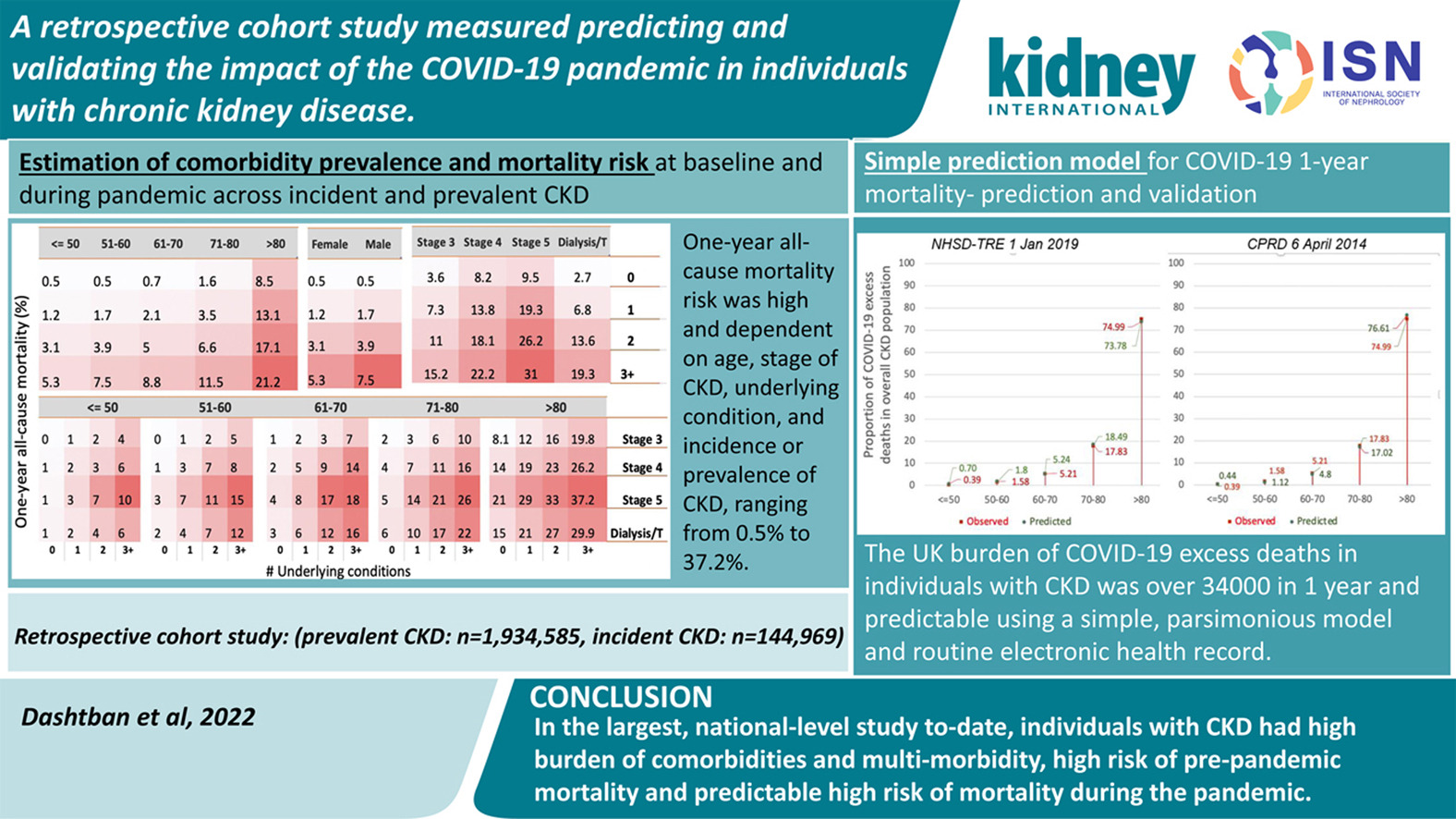
The results, published in the journal Kidney International, show that two-thirds of the patients had at least one other condition, such as high blood pressure or heart disease, that put them at moderate or high risk of dying from COVID-19.
“Kidney disease has been understudied in large datasets,” says Professor Banerjee. “Our findings highlight the complexity of chronic kidney disease and linked health conditions that people living with kidney disease have to face. We are trying to use electronic health records to provide the most relevant personalised information that we can so that we are in the best position to treat and support patients and improve their quality of life.”
Largest ever study
The team validated their model using health records from 56 million people in England, accessed safely and securely through the NHS Digital Trusted Research Environment. This was linked to data on deaths related to COVID-19 between 1 March 2020 and 1 March 2021.
By identifying the risk faced by each patient, the researchers could predict the increased number of deaths during the pandemic. Their model predicted up to 23,754 additional deaths in people with chronic kidney disease over one year, underestimating the real figure of 34,265 mostly because of a high direct and indirect impact of the pandemic on diabetes and cancer patients.
Dr Muhammad Dashtban, a data scientist at UCL who led the study, said: “People living with chronic kidney disease in the UK have a high burden of other health issues. We hope that our findings could be used to devise guidelines or treatment strategies for different subgroups that could help to develop personalised health care.”
Not an equal risk
The health records were also examined for the severity of kidney disease. This was one of the major contributing factors that influenced the number of deaths observed, together with age, sex and diagnosis of other conditions.
“There hasn’t been a national-level study with this level of granularity about comorbidities and all the different risks over one year. It shows that not all people with kidney disease are equal in their risk,” says Professor Banerjee.
The BHF Data Science Centre worked with NHS Digital to co-develop the platform to access the de-identified health records and combine them across systems.
Professor Cathie Sudlow, Director of the BHF Data Science Centre, said: “This study is the first time that large-scale routine health records have been used to understand the impact of chronic kidney disease in the context of COVID-19. Importantly, using this data could predict excess deaths and help policymakers act accordingly.”
You can read the original paper here.



