Realising the potential of Learning Health Systems for Better Care
9 July 2021 | Author: Dr Tom Foley, Senior Clinical Lead for Data
The HDR UK Better Care Programme was founded on one clear vision: that patients across the UK will benefit from largescale data and advanced analytics, identifying what works best for them.
At the outset, the Health Foundation funded the Learning Healthcare Project at Newcastle University to investigate how local, regional, national and international organisations can realise the Better Care Programme’s vision by becoming Learning Health Systems. We have now published our report.
HDR UK developed the Better Care Loop which describes the technical building blocks required to support a Learning Health System.
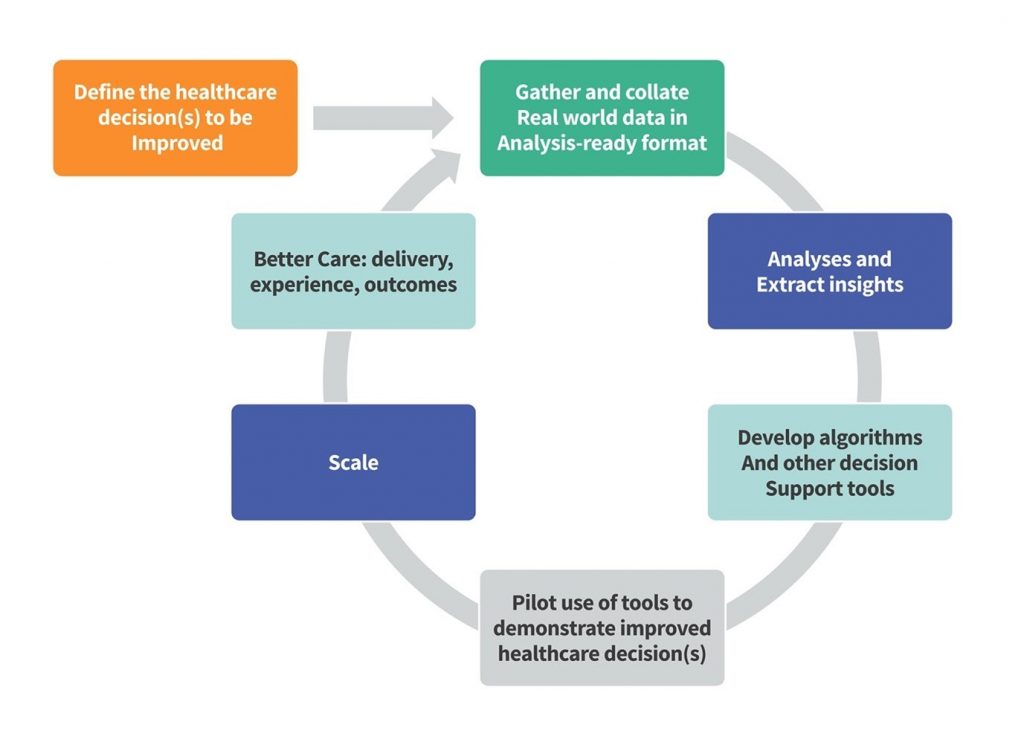
We adopted a high-level version of this loop with three key elements: Practice to Data, Data to Knowledge and Knowledge to Practice. The Better Care Programme and HDR UK more broadly have already made huge progress in each of these areas, but our review of the literature, our workshops, our interviews and our personal experience told us that we needed a broad framework to support those technical building blocks.

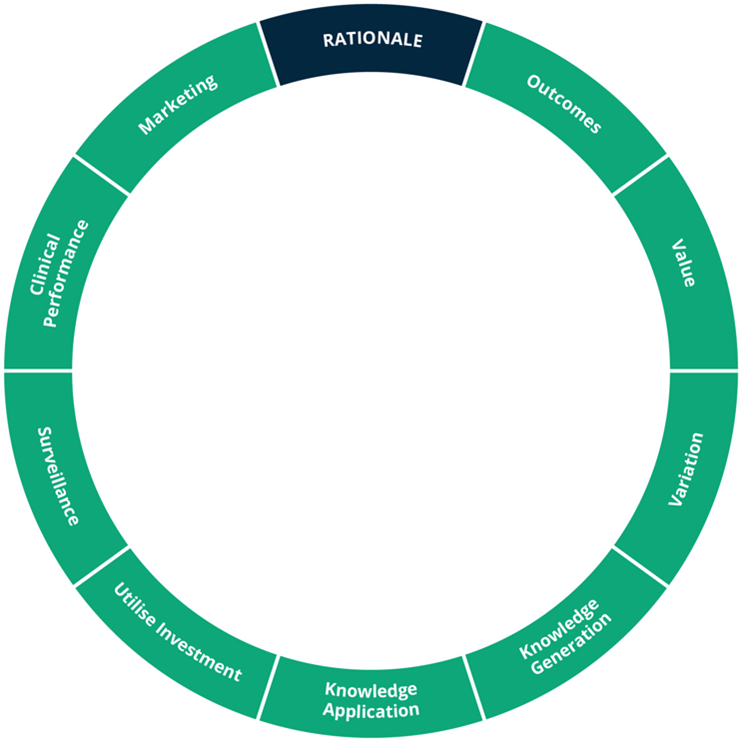
First, we need to understand why we are building a Learning Health System. This will be different for each organisation. It could be to enhance outcomes and experience for patients, to improve value, reduce variation, to generate new knowledge, to apply existing knowledge, to make better use of our IT investments or to boost clinical performance.
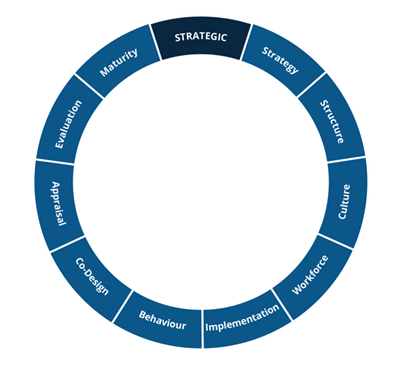
Once we understand the rationale, the whole organisation(s) must be aligned around a strategic direction, with the structures in place to deliver it. We must create a culture of learning and take a scientific approach to implementation. We must change behaviour and continually evaluate our progress. All of this must be co-designed with our patients, colleagues and key stakeholders.
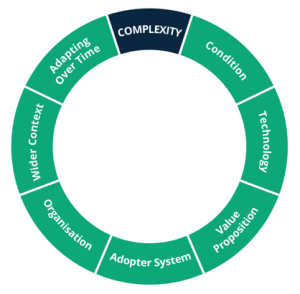
A Learning Health System is likely to comprise many initiatives and complexity is a key source of failure. In order to understand the complexity within and between these initiatives, we integrated the Non-adoption, Abandonment, and challenges to Scale-up, Spread and Sustainability (NASSS) Framework.
Often the illness is more complex than assumed, with challenging co-morbidities or socioeconomic associations that the system can’t handle. Often the value proposition doesn’t make sense for the organisations involved. Often those organisations are under too much pressure or have limited capacity for innovation. On many occasions, we have unrealistic expectations of the patients, carers and clinicians who will actually use the system. The outside world can also intervene with regulations or political realities that challenge the project. And even if you overcome all these, any individual element could still change over time.
 We brought all of these components together into an overarching framework.
We brought all of these components together into an overarching framework.
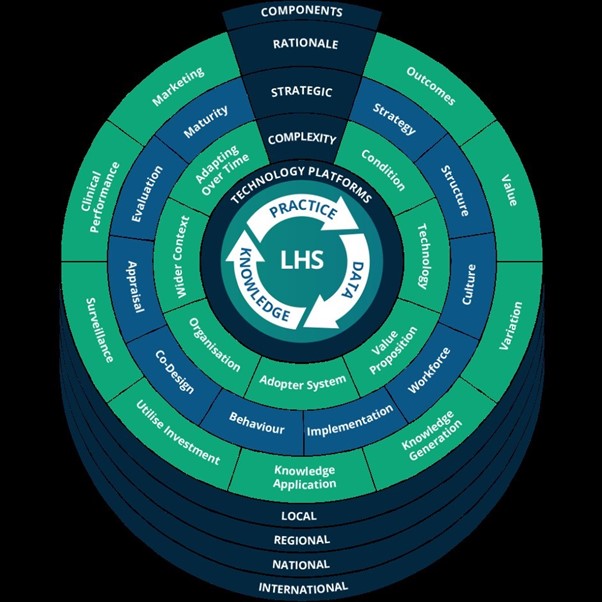 In keeping with the Learning Health System philosophy, this framework is not the final word. It is a starting point. We are now working – and collaborating internationally – to turn the framework and our report into an online toolkit that will evolve over time, based on contributions from Better Care Programme participants and the global Learning Health System community.
In keeping with the Learning Health System philosophy, this framework is not the final word. It is a starting point. We are now working – and collaborating internationally – to turn the framework and our report into an online toolkit that will evolve over time, based on contributions from Better Care Programme participants and the global Learning Health System community.



