Improving hospital operational efficiency by forecasting demand for hospital beds
This project aims to utilise live care data to forecast emergency hospital admissions, demand for beds and theatres, and to plan elective surgery accordingly. This will enable trusts to better plan their resource allocations and reduce A&E crowding.
The Challenge
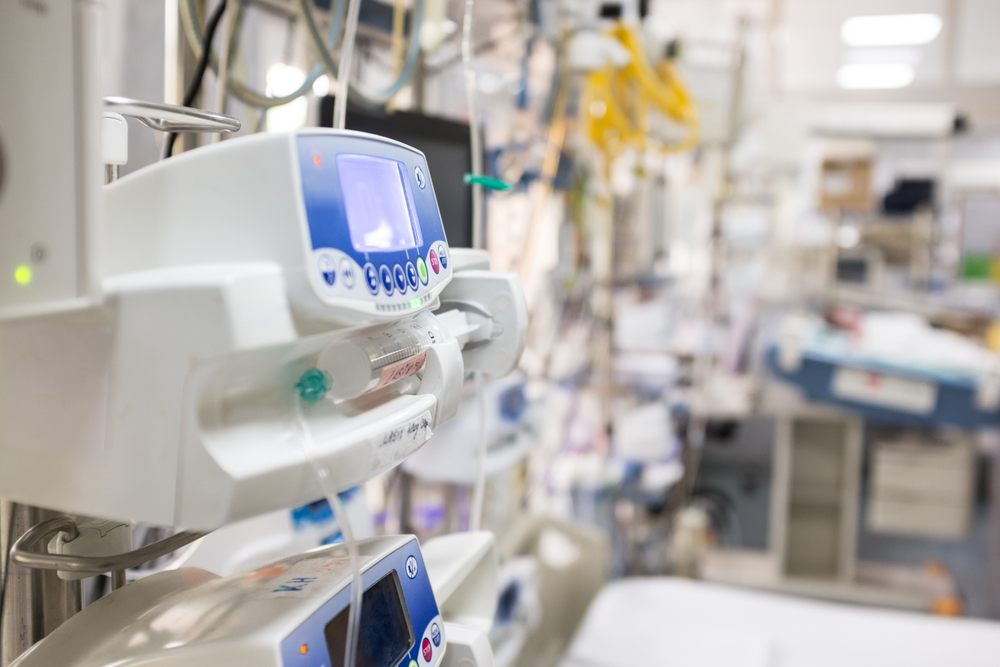
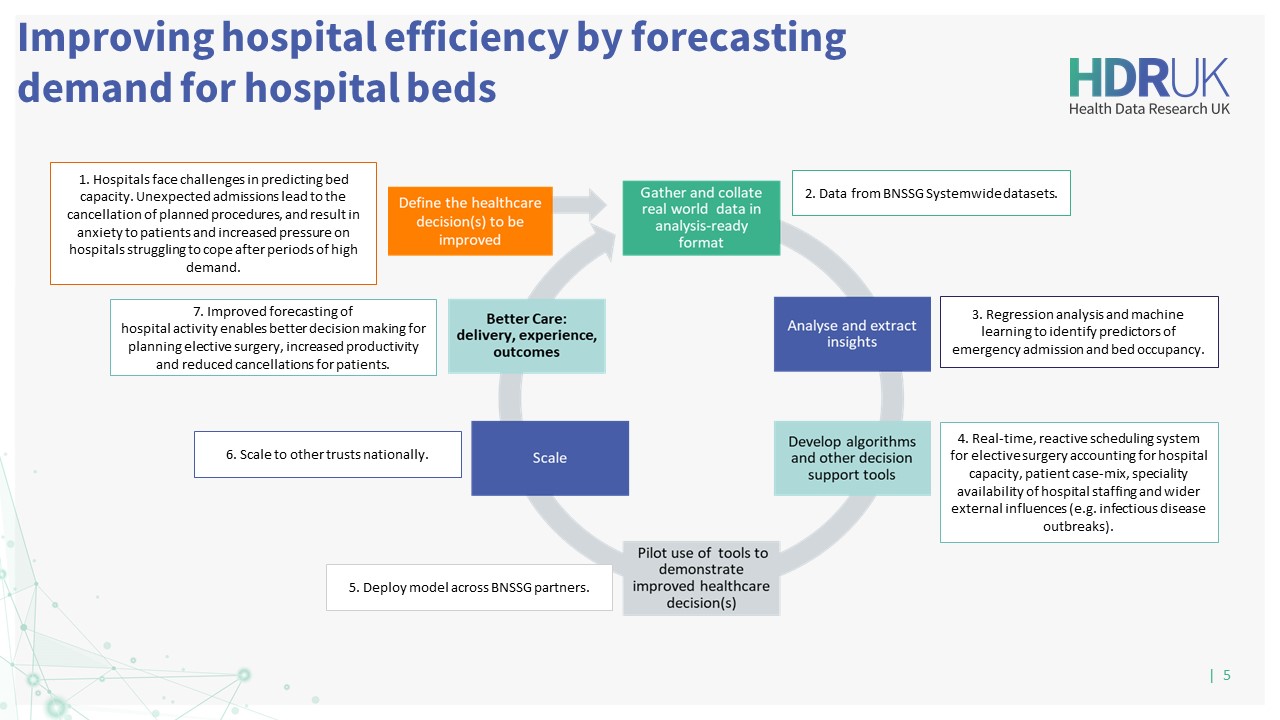
NHS acute hospital trusts face challenges in planning hospital bed capacity, especially in winter months when patient demand for hospital care is high. Hospital service managers need to be able to plan ahead, and proactively monitor demand for hospital beds and operating theatres.
Efficient allocation of beds, staff and funding has become an urgent issue for many hospital administrations, particularly due to the rising number of people admitted as emergency cases. The increase in the number of unpredicted hospital admissions has led to the cancellation of planned procedures and operations, causing worry and anxiety to patients. It also causes increased pressure on hospitals as they cope with rescheduled procedures after periods of high demand.
The Solution
Care computer systems containing live information relating to patients, staffing, theatres and beds could be used to manage patient demand for hospital beds. These data can be used to forecast emergency hospital admissions, demand for beds and theatres, and to plan elective surgery accordingly. The team will use existing local datasets and methodologies from economics and statistics, to develop algorithms that will predict patient demand for hospital beds.
The Impact and Outcomes
Improved modelling of demand will have a direct impact on the business planning of acute NHS Trusts. By understanding patient volume, trusts can plan what the optimal resource allocation to meet that demand, including the number of beds required, the workforce and the theatre time on any given day. This in turn will provide insight into the remaining capacity available for elective work.
Improving patient flow through hospitals greatly improves the working and care environment, reduces A&E crowding, avoids last-minute cancellations of elective procedures and enables hospitals to provide the most appropriate care for patients.
Better Care Loop
Project Team
Prof Ashley Blom, Professor of Orthopaedic Surgery and Head of Bristol Medical School
Prof Andrew Judge, Professor of Translational Statistics, Department of Translational Health Sciences, Bristol Medical School, University of Bristol