The Land War in the fight against COVID
3 November 2020 | Author: Peter Diggle, Former Director of the HDRUK-Turing Wellcome PhD Programme in Health Data Science
Peter Diggle (Health Data Research UK), Richard Lilford, Sam Watson (University of Birmingham)
If it wasn’t so before last weekend, it is now…gone are the days of thinking there is a quick fix to the COVID-19 pandemic. Another country-wide lockdown should reduce COVID-19 infection, but at the same time will damage the economy and pose a threat to other long-term health conditions, with disproportionate effects on the more disadvantaged groups in society. The Great Barrington Declaration – aiming for herd immunity while sequestering high-risk people – does not bear close examination.[1] Vaccination is not an automatic get out of jail card – we do not yet know when vaccination will be available at the required volume, nor what degree of protection it will confer. So, this is the land war. We must work on supply chains, procedures, detection and contact tracing, getting ever slicker at the operation. Personal protection, social distancing and graded lockdowns can all play a part, but only if they are accepted by the general public, who deserve clear explanations of when, where and why unwelcome restrictions will be imposed and what these restrictions are intended to achieve.
While central government has an obvious role to play, it has become clear that the battle must go local; and the more local the better. The risk of being hospitalised with COVID-19 in Birmingham varies dramatically across the various electoral wards, with the seven-day rolling rate of new cases (for week ending 14 October 2020) ranging from 43.8 per 100,000 in Nechells, to 825.8 in Selly Oak.[2] So, supported by the MRC, NIHR ARC West Midlands and our3] host hospital (University Hospitals Birmingham NHS Foundation Trust) we are developing a computer application to track the evolving pattern of the COVID-19 pandemic.
We have developed software that uses geospatial statistical models[3] to identify “hot spots”, however one defines them, across a broad space such as an urban conurbation or a country. Within such a space we identify localities at whatever scale is relevant for local decision-making and that the data can support. We can map rates of infection per unit of population in real time on these maps to show the current state of the epidemic and its direction of travel (see Example below). These maps can direct decision-makers to specific localities where incidence is increasing rapidly and hence where urgent action is needed.
But there is a problem with policy action directed at small areas and particular communities – dictatorial edicts are likely to provoke resentment rather than effective action, especially when carried out at a very local level. It is one thing to place restrictions across a whole country or even a large city, but quite another to try to lockdown an area such as Lady Pool in Birmingham or Chapel Town in Leeds. Indeed, the disease has highest incidence in BAME communities who may feel victimised or disenfranchised. Already only 18% of people fully comply with UK regulations regarding self-isolation.[4] So here we come to the second use of our software and the maps it produces.
We think that policy-makers should increasingly turn to local communities and ask them to be the architects, not recipients, of policy. In essence we are arguing for an ‘assets-based’ or ‘participatory’ approach based on ‘co-invention’. And here our software can help by providing scientific data at a local level in a form that can be easily assimilated. There is evidence that populations relate well to local maps and they are sometimes used in qualitative research as a method to promote discussion among people.[5]
Example: Real-Time Surveillance of COVID-19
For this example we have aggregated the results to MSOA (middle-layer Super Output Area) level across the catchment area of University Hospitals Birmingham NHS Foundation Trust, although we have retained other areas of Birmingham to make the boundary of the city clear. One could aggregate to smaller or larger levels as needed.
We have produced these outputs as if we were working on March 26 2020 using data from the preceding two weeks. The first thing someone interested in tracking COVID-19 in the city might ask is what is the incidence of the disease that day?
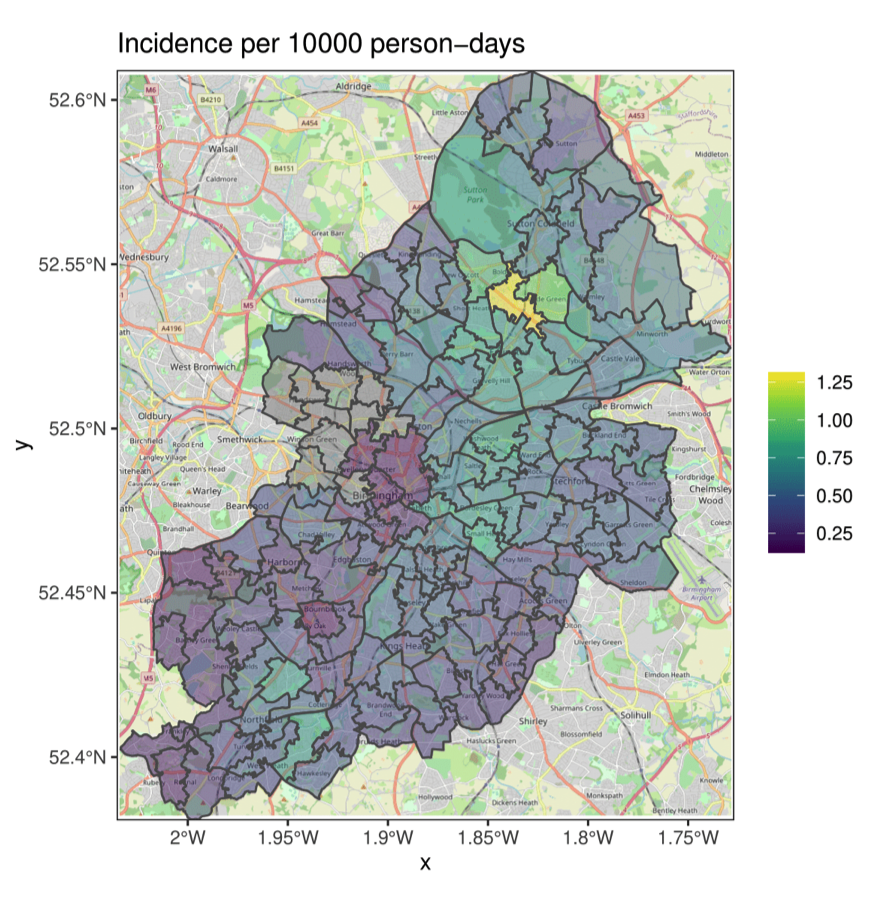
There is a lot of variation across the different MSOAs, with one area standing out as being high (yellow area). The variation here could be explained by differences in demographics or socioeconomic status, and we might want to ask whether any differences are for unexpected reasons. To do this, we need to break down the incidence into different components:
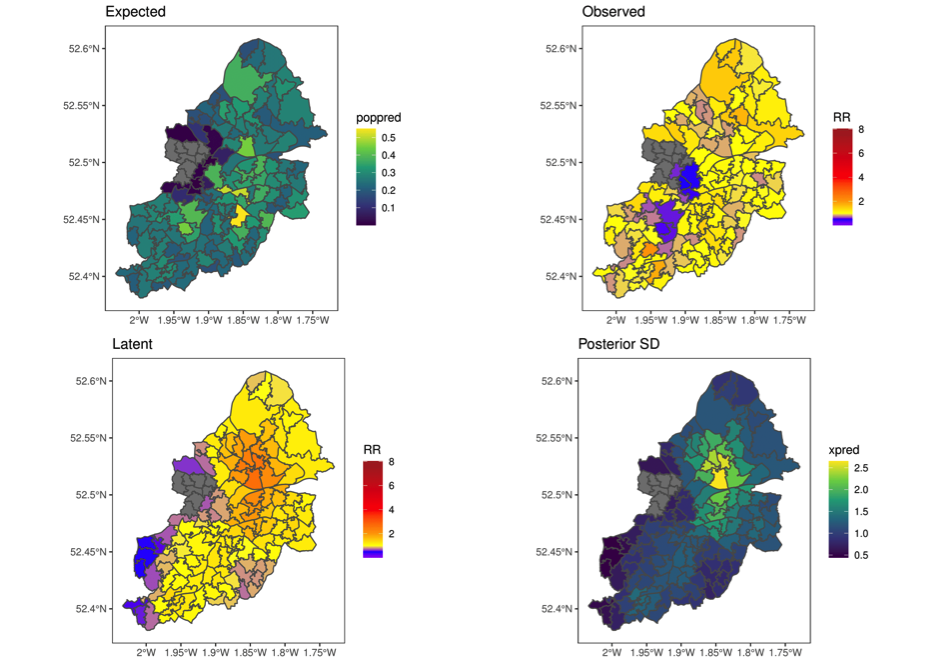
In this four-panel display:
- Expected is the number of cases we would expect that day from each area based on the size of its population, if risk does not vary by location.
- Observed shows the relative risk in each area associated with observable characteristics (age, ethnicity, and deprivation). For example, if the average incidence across the city were one case per 10,000 person-days, an area with a larger proportion of older residents would have a high risk; if this risk were double the average then it would have a relative risk of two.
- Latent is the relative risk in each area not explained by its observable characteristics. Our area with more older people may have an expected incidence of two cases per 10,000 person-days (a ‘baseline’ of 1 per 10,000 person-days times a relative risk of 2), but if unobserved characteristics confer a further 50% increase in risk, this results in an average rate of 3 (1 times 2 times 1.5) cases per 10,000 person-days,
- Posterior SD indicates the standard deviation, a statistical measure of the uncertainty around each prediction
Based on these plots the area in the North of Birmingham coloured orange in the bottom-left plot has a level of risk higher than can be explained by its observed characteristics by a factor of 2 or 3. This may indicate the need for a local public health intervention.
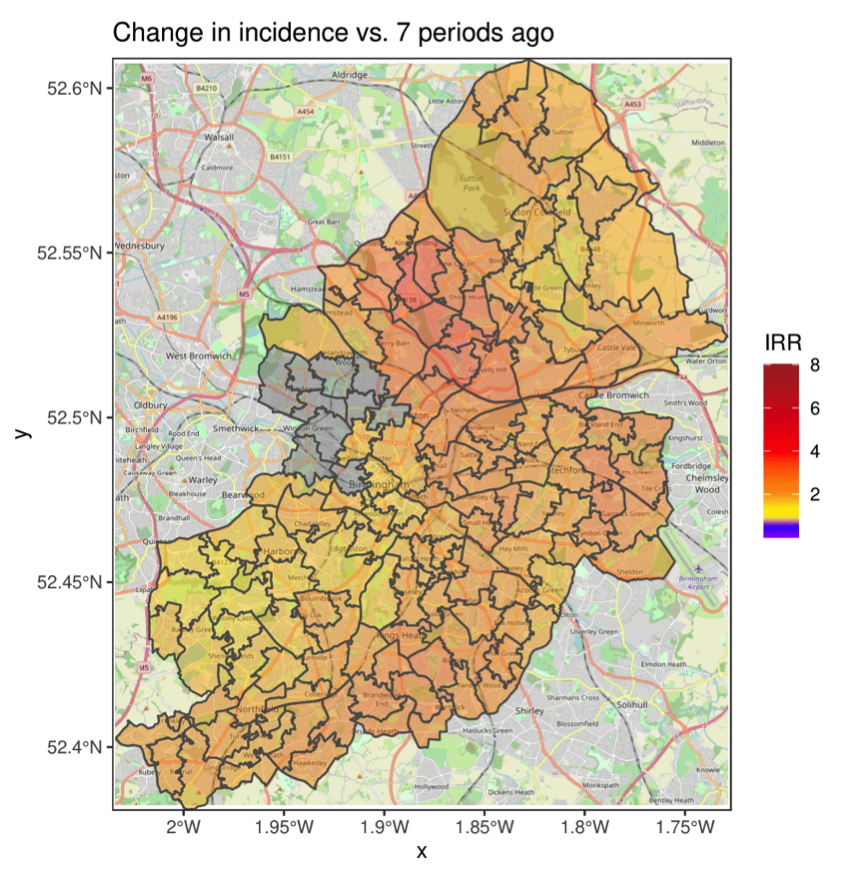
We might finally ask, how does this day’s risk map compare with the map for the same day last week? The next plot shows the incidence rate ratio, which here is the ratio of incidence compared to seven days prior for each area. A value of one indicates no change, two a doubling, and so forth. One can clearly see that it is above one, i.e. risk is increasing, city-wide. The greatest relative increases are centred on the north-central area we identified above as being of high concern.
References:
- Alwan NA, Burgess RA, Ashworth S, et al. Scientific consensus on the COVID-19 pandemic: we need to act now. Lancet. 2020.
- Public Health England. Coronavirus (COVID-19) in the UK: Interactive Map. 19 October 2020
- Diggle, PJ, Rowlingson, B and Su, T-L Point process methodology for on-line spatio-temporal disease surveillance. 2005
- Smith LE, Potts HWW, Amlot R, et al. Adherence to the test, trace and isolate system: results from a time series of 21 nationally representative surveys in the UK (the COVID-19 Rapid Survey of Adherence to Interventions and Responses [CORSAIR] study). MedRXiv. 2020. [Pre-print].
- Boschmann EE, Cubbon E. Sketch maps and qualitative GIS: Using cartographies of individual spatial narratives in geographic research. Professional Geographer. 2014;66(2):236-48.